January 2024 –
Flu At A Glance
CAUSED BY:
Influenza, or flu, is an illness caused by a virus transmitted through tiny droplets of moisture, created when people with flu cough, sneeze, or even talk. Since there’s no better time to catch up with everyone than over the holidays, this unfortunately means that it has plenty of opportunity to jump from person to person.
SPREAD BY:
The flu virus is very contagious and can be spread by someone that has the flu from the day before they start to feel symptoms, up to seven days afterwards. Regardless of how careful people with the illness can be, these viruses settle and accumulate on door handles, gadgets and most importantly: kitchen surfaces. It’s a cruel joke that the flu season falls over the time of year with the best food!
SYMPTOMS INCLUDE:
- Cough
- Sore throat
- Muscle aches and pains
- Runny or stuffy nose
Lots of people associate flu with having a fever, and whilst this can be a nasty symptom, not everyone with flu gets it, so don’t rule it out even if you don’t have this symptom yourself.
LASTS FOR:
Although most people get over the worst of the flu in a week or so, it can be very unpredictable and certain people are at greater risk of serious complications, particularly young children and the elderly.
Lets do our part and protect ourselves as well as our elderly population. Wash your hands often, cough into your elbow, clean surfaces with a Clorox mix or something similar to kill the germs.
9/2023 – A new strain of Covid which is causing concern among scientists due to its high number of mutations has been confirmed in four cases in the UK.
The variant, named Pirola, was already detected in a number of countries before arriving here, with experts worried that it could have the capacity to evade immunity from vaccinations or previous infections.
What is Pirola, does it cause more severe illness, and will the vaccine hold up against it?
Pirola – also known as BA.2.86 – has been named by scientists after ‘an asteroid that hangs out near Jupiter’.
It is a subvariant of the Omicron strain which descends from the BA.2 variant, which led to widespread cases at the start of 2022.
It’s said to have over 30 mutations to its spike protein – the part of the virus that allows it to invade human cells – which has raised fears that it could evade current treatments and vaccines, as well as natural immunity to infection from a previous bout of Covid.
‘Interestingly, all 30-plus mutations on that long branch are found in the spike protein—through which the virus gains entry to cells—which is the target of neutralising antibodies.’
The variant was first detected in Denmark on July 24, and has since been confirmed in a number of countries including South Africa, Canada, Denmark, Sweden, Israel and the US.
The confirmed case in the UK came from a person who had no recent history of travel, indicating that it may be spreading here – although it’s still unclear whether it could be more infectious than previous strains.
‘More data are needed to understand this Covid-19 variant and the extent of its spread,’ the World Health Organization said.
At this stage it’s not yet known whether Pirola causes different symptoms to other Covid variants.
a high temperature or shivering (chills)
a new, continuous cough – this means coughing a lot for more than an hour, or 3 or more coughing episodes in 24 hours.
a loss or change to your sense of smell or taste.
shortness of breath
feeling tired or exhausted
an aching body
a headache
a sore throat
a blocked or runny nose
loss of appetite
diarrhea
feeling sick or being sick
If you test positive for Covid current NHS advice is to try and stay at home for five days and avoid, contact with other people.
You should call NHS 111 if your symptoms or those of a child’s are getting worse rather than better – and in the event of an emergency such as severe breathlessness, coughing up blood or collapsing, you should dial 999 or go to A&E.
It’s not yet known whether Pirola causes more severe illness than other strains of Covid.
Once again, it’s too early to say whether current vaccines and treatments will work against Pirola.
However, the Center for Disease Control in the US has noted that existing tests and treatments appear to be effective against the new variant.
WESTERN MONTANA AREA VI AGENCY ON AGING, INC.
COVID-19 COMMUNITY RESOURCE LIST
January 24, 2023 CDC Update to Covid-19 Testing and Treatment for current SARS-Cov-2 Variants
As SARS-CoV-2 variants evolve, circulating variants have increased transmissibility and ability to evade the immune system, which changes the treatment and prevention options for COVID-19. Clinicians should understand the nuances of current SARS-CoV-2 testing and treatment to prevent hospitalizations and deaths among people at high risk of severe disease.
During this COCA Call, subject matter experts will provide an overview of COVID-19 epidemiology and the current variant landscape, address current Centers for Disease Control and Prevention testing guidance and the National Institutes of Health and Infectious Disease Society of America COVID-19 treatment guidelines, and discuss risk assessment and considerations for treatment options.
As of January 26, 2023, EVUSHELDTM is not currently authorized for emergency use because it is unlikely to be active against the majority of SARS-CoV-2 variants circulating in the United States.
- If you are moderately or severely immunocompromised (have a weakened immune system), you are at increased risk of severe COVID-19 illness and death. Additionally, your immune response to COVID-19 vaccination may not be as strong as in people who are not immunocompromised.
- As with vaccines for other diseases, you are protected best when you stay up to date with your COVID-19 vaccines for your age group:
- COVID-19 vaccine and booster recommendations may be updated as CDC continues to monitor the latest COVID-19 data.
Who Is Moderately or Severely Immunocompromised?
Some people are immunocompromised (have a weakened immune system) due to a medical condition or from receipt of immunosuppressive medications or treatments. Learn more about which medical conditions put you at increased risk of severe COVID-19 illness and death. You can self-attest to your moderately or severely immunocompromised status, which means you do not need any documentation of your status to receive COVID-19 vaccine doses you might be eligible to receive.
People Who Were Vaccinated Outside of the United States
People who are moderately or severely immunocompromised and who received COVID-19 vaccines not available in the United States should either complete or restart the recommended COVID-19 vaccine series, including a booster, in the United States. For more information, talk to your healthcare provider, or see the COVID-19 Interim Clinical Considerations.
Availability:
• As of 07/27/2022, 750 doses of Jynneos have been allocated to Montana, 390 of which are currently accessible.
o An additional 180 of doses will be available Aug 15th
For more information visit –> https://dphhs.mt.gov/publichealth/cdepi/diseases/monkeypox
MonkeyPox July 11 2022 CDC update
Monkeypox is a rare disease caused by infection with the monkeypox virus. Monkeypox virus is part of the same family of viruses as variola virus, the virus that causes smallpox. Monkeypox symptoms are similar to smallpox symptoms, but milder, and monkeypox is rarely fatal. Monkeypox is not related to chickenpox.
Monkeypox was discovered in 1958 when two outbreaks of a pox-like disease occurred in colonies of monkeys kept for research. Despite being named “monkeypox,” the source of the disease remains unknown. However, African rodents and non-human primates (like monkeys) might harbor the virus and infect people.
The first human case of monkeypox was recorded in 1970. Prior to the 2022 outbreak, monkeypox had been reported in people in several central and western African countries. Previously, almost all monkeypox cases in people outside of Africa were linked to international travel to countries where the disease commonly occurs or through imported animals. These cases occurred on multiple continents.
Monkeypox Symptoms
Monkeypox is a rare disease caused by infection with the monkeypox virus. Monkeypox virus is part of the same family of viruses as smallpox. Monkeypox symptoms are similar to smallpox symptoms, but milder; and monkeypox is rarely fatal. Monkeypox is not related to chickenpox.
Symptoms of monkeypox can include:
- Fever
- Headache
- Muscle aches and backache
- Swollen lymph nodes
- Chills
- Exhaustion
- A rash that can look like pimples or blisters that appears on the face, inside the mouth, and on other parts of the body, like the hands, feet, chest, genitals, or anus.
The rash goes through different stages before healing completely. The illness typically lasts 2-4 weeks. Sometimes, people get a rash first, followed by other symptoms. Others only experience a rash.
Take the following steps to prevent getting monkeypox:
- Avoid close, skin-to-skin contact with people who have a rash that looks like monkeypox.
- Do not touch the rash or scabs of a person with monkeypox.
- Do not kiss, hug, cuddle or have sex with someone with monkeypox.
- Do not share eating utensils or cups with a person with monkeypox.
- Do not handle or touch the bedding, towels, or clothing of a person with monkeypox.
- Wash your hands often with soap and water or use an alcohol-based hand sanitizer.
- In Central and West Africa, avoid contact with animals that can spread monkeypox virus, usually rodents and primates. Also, avoid sick or dead animals, as well as bedding or other materials they have touched.
If you are sick with monkeypox:
- Isolate at home
- If you have an active rash or other symptoms, stay in a separate room or area away from people or pets you live with, when possible.
Vaccination
CDC recommends vaccination for people who have been exposed to monkeypox and people who are at higher risk of being exposed to monkeypox, including:
- People who have been identified by public health officials as a contact of someone with monkeypox
- People who may have been exposed to monkeypox, such as:
- People who are aware that one of their sexual partners in the past 2 weeks has been diagnosed with monkeypox
- People who had multiple sexual partners in the past 2 weeks in an area with known monkeypox
- People whose jobs may expose them to orthopoxviruses, such as:
- Laboratory workers who perform testing for orthopoxviruses
- Laboratory workers who handle cultures or animals with orthopoxviruses
- Some designated healthcare or public health workers
March 2022 – A new CDC MMWR found that when the Omicron variant was widely circulating, rates of COVID-19-associated hospitalization increased for all adults, regardless of vaccination status.
Everyone eligible should stay up to date with their COVID-19 vaccinations, including booster doses, to reduce their risk for severe COVID-19. Learn more: bit.ly/MMWR7112e2.
CDC Updates and Shortens Recommended Isolation and Quarantine Period for General Population
For Immediate Release: Monday, December 27, 2021
Given what we currently know about COVID-19 and the Omicron variant, CDC is shortening the recommended time for isolation from 10 days for people with COVID-19 to 5 days, if asymptomatic, followed by 5 days of wearing a mask when around others. The change is motivated by science demonstrating that the majority of SARS-CoV-2 transmission occurs early in the course of illness, generally in the 1-2 days prior to onset of symptoms and the 2-3 days after. Therefore, people who test positive should isolate for 5 days and, if asymptomatic at that time, they may leave isolation if they can continue to mask for 5 days to minimize the risk of infecting others.
Additionally, CDC is updating the recommended quarantine period for those exposed to COVID-19. For people who are unvaccinated or are more than six months out from their second mRNA dose (or more than 2 months after the J&J vaccine) and not yet boosted, CDC now recommends quarantine for 5 days followed by strict mask use for an additional 5 days. Alternatively, if a 5-day quarantine is not feasible, it is imperative that an exposed person wear a well-fitting mask at all times when around others for 10 days after exposure. Individuals who have received their booster shot do not need to quarantine following an exposure but should wear a mask for 10 days after the exposure. For all those exposed, best practice would also include a test for SARS-CoV-2 at day 5 after exposure. If symptoms occur, individuals should immediately quarantine until a negative test confirms symptoms are not attributable to COVID-19.
Isolation relates to behavior after a confirmed infection. Isolation for 5 days followed by wearing a well-fitting mask will minimize the risk of spreading the virus to others. Quarantine refers to the time following exposure to the virus or close contact with someone known to have COVID-19. Both updates come as the Omicron variant continues to spread throughout the U.S. and reflects the current science on when and for how long a person is maximally infectious.
Data from South Africa and the United Kingdom demonstrate that vaccine effectiveness against infection for two doses of an mRNA vaccine is approximately 35%. A COVID-19 vaccine booster dose restores vaccine effectiveness against infection to 75%. COVID-19 vaccination decreases the risk of severe disease, hospitalization, and death from COVID-19. CDC strongly encourages COVID-19 vaccination for everyone 5 and older and boosters for everyone 16 and older. Vaccination is the best way to protect yourself and reduce the impact of COVID-19 on our communities.
If You test positive:
Everyone, regardless of vaccination status.
- Stay home for 5 days.
- If you have no symptoms or your symptoms are resolving after 5 days, you can leave your house.
- Continue to wear a mask around others for 5 additional days.
If you have a fever, continue to stay home until your fever resolves.
If You have been exposed to Covid-19:
If you:
Have been boosted
OR
Completed the primary series of Pfizer or Moderna vaccine within the last 6 months
OR
Completed the primary series of J&J vaccine within the last 2 months
- Wear a mask around others for 10 days.
- Test on day 5, if possible.
If you develop symptoms get a test and stay home.
Omicron
A new variant of SARS-CoV-2 (the virus that causes COVID-19), B.1.1.529 (Omicron) (1), was first reported to the World Health Organization (WHO) by South Africa on November 24, 2021. Omicron has numerous mutations with potential to increase transmissibility, confer resistance to therapeutics, or partially escape infection- or vaccine-induced immunity (2). On November 26, WHO designated B.1.1.529 as a variant of concern (3), as did the U.S. SARS-CoV-2 Interagency Group (SIG)* on November 30. On December 1, the first case of COVID-19 attributed to the Omicron variant was reported in the United States. As of December 8, a total of 22 states had identified at least one Omicron variant case, including some that indicate community transmission. Among 43 cases with initial follow-up, one hospitalization and no deaths were reported. This report summarizes U.S. surveillance for SARS-CoV-2 variants, characteristics of the initial persons investigated with COVID-19 attributed to the Omicron variant and public health measures implemented to slow the spread of Omicron in the United States. Implementation of concurrent prevention strategies, including vaccination, masking, increasing ventilation, testing, quarantine, and isolation, are recommended to slow transmission of SARS-CoV-2, including variants such as Omicron, and to protect against severe illness and death from COVID-19.
Measures to Slow Domestic Spread of the Omicron Variant
CDC recommends prioritizing case investigation and contact tracing††† for confirmed COVID-19 cases attributed to the Omicron variant. This prioritization should be balanced with maintaining case investigation and contact tracing for outbreaks of confirmed cases of SARS-CoV-2 infection in high-risk congregate settings (e.g., long-term care facilities, correctional facilities, and homeless shelters) and for persons at increased risk for severe COVID-19–related health outcomes. Timely case investigation and contact tracing can help ensure compliance with isolation and quarantine guidance§§§ and link persons with positive SARS-CoV-2 test results and their close contacts to testing and supportive services.
What We Know about Omicron
Infection and Spread
- How easily does Omicron spread? The Omicron variant likely will spread more easily than the original SARS-CoV-2 virus and how easily Omicron spreads compared to Delta remains unknown. CDC expects that anyone with Omicron infection can spread the virus to others, even if they are vaccinated or don’t have symptoms.
- Will Omicron cause more severe illness? More data are needed to know if Omicron infections, and especially reinfections and breakthrough infections in people who are fully vaccinated, cause more severe illness or death than infection with other variants.
- Will vaccines work against Omicron? Current vaccines are expected to protect against severe illness, hospitalizations, and deaths due to infection with the Omicron variant. However, breakthrough infections in people who are fully vaccinated are likely to occur. With other variants, like Delta, vaccines have remained effective at preventing severe illness, hospitalizations, and death. The recent emergence of Omicron further emphasizes the importance of vaccination and boosters.
- Will treatments work against Omicron? Scientists are working to determine how well existing treatments for COVID-19 work. Based on the changed genetic make-up of Omicron, some treatments are likely to remain effective while others may be less effective.
We have the Tools to Fight Omicron
Vaccines remain the best public health measure to protect people from COVID-19, slow transmission, and reduce the likelihood of new variants emerging. COVID-19 vaccines are highly effective at preventing severe illness, hospitalizations, and death. Scientists are currently investigating Omicron, including how protected fully vaccinated people will be against infection, hospitalization, and death. CDC recommends that everyone 5 years and older protect themselves from COVID-19 by getting fully vaccinated. CDC recommends that everyone ages 18 years and older should get a booster shot at least two months after their initial J&J/Janssen vaccine or six months after completing their primary COVID-19 vaccination series of Pfizer-BioNTech or Moderna.
Masks offer protection against all variants. CDC continues to recommend wearing a mask in public indoor settings in areas of substantial or high community transmission, regardless of vaccination status. CDC provides advice about masks for people who want to learn more about what type of mask is right for them depending on their circumstances.
Tests can tell you if you are currently infected with COVID-19. Two types of tests are used to test for current infection: nucleic acid amplification tests (NAATs) and antigen tests. NAAT and antigen tests can only tell you if you have a current infection. Individuals can use the COVID-19 Viral Testing Tool to help determine what kind of test to seek. Additional tests would be needed to determine if your infection was caused by Omicron. Visit your state, tribal, local, or territorial health department’s website to look for the latest local information on testing.
Self-tests can be used at home or anywhere, are easy to use, and produce rapid results. If your self-test has a positive result, stay home or isolate for 10 days, wear a mask if you have contact with others, and call your healthcare provider. If you have any questions about your self-test result, call your healthcare provider or public health department.
Until we know more about the risk of Omicron, it is important to use all tools available to protect yourself and others.
Some COVID-19 Vaccine Recipients Can Get Booster Shots
- People 65 years and older, 50–64 years with underlying medical conditions, or 18 years and older who live in long-term care settings should receive a booster shot.
- People 18 years and older should receive a booster shot at least 2 months after receiving their Johnson & Johnson/Janssen COVID-19 vaccine.
-
IF YOU RECEIVED
Pfizer-BioNTech or Moderna
You are eligible for a booster if you are:
- 65 years or older
- Age 18+ who live in long-term care settings
- Age 18+ who have underlying medical conditions
- Age 18+ who work or live in high-risk settings
When to get a booster:
At least 6 months after your second shotWhich booster should you get?
Any of the COVID-19 vaccines authorized in the United States -
IF YOU RECEIVED
Johnson & Johnson’s Janssen
You are eligible for a booster if you are:
18 years or olderWhen to get a booster:
At least 2 months after your second shotWhich booster should you get?
Any of the COVID-19 vaccines authorized in the United States -
Choosing Your COVID-19 Booster Shot
You may choose which COVID-19 vaccine you receive as a booster shot. Some people may have a preference for the vaccine type that they originally received, and others may prefer to get a different booster. CDC’s recommendations now allow for this type of mix and match dosing for booster shots.
-
IF YOU RECEIVED
Pfizer-BioNTech or Moderna COVID-19 Vaccine
Older adults age 65 years and older
People ages 65 years and older should get a booster shot. The risk of severe illness from COVID-19 increases with age and can also increase for adults of any age with underlying medical conditions.
Long-term care setting residents ages 18 years and older
Residents ages 18 years and older of long-term care settings should get a booster shot. Because residents in long-term care settings live closely together in group settings and are often older adults with underlying medical conditions, they are at increased risk of infection and severe illness from COVID-19.
People with underlying medical conditions ages 50–64 years
People ages 50–64 years with underlying medical conditions should get a booster shot. The risk of severe illness from COVID-19 increases with age and can also increase for adults of any age with underlying medical conditions.
People with underlying medical conditions ages 18–49 years
People ages 18–49 years with underlying medical conditions may get a booster shot based on their individual risks and benefits. The risk of severe illness from COVID-19 can increase for adults of any age with underlying medical conditions. This recommendation may change in the future as more data become available.
People who work or live in high-risk settings ages 18–64 years
People ages 18–64 years at increased risk for COVID-19 exposure and transmission because of occupational or institutional setting may get a booster shot based on their individual risks and benefits. Adults who work or reside in certain settings (e.g., health care, schools, correctional facilities, homeless shelters) may be at increased risk of being exposed to COVID-19, which could be spreading where they work or reside. That risk can vary across settings and based on how much COVID-19 is spreading in a community. This recommendation may change in the future as more data become available.
Examples of workers who may get COVID-19 booster shots: [ 1 ]
- First responders (e.g., healthcare workers, firefighters, police, congregate care staff)
- Education staff (e.g., teachers, support staff, daycare workers)
- Food and agriculture workers
- Manufacturing workers
- Corrections workers
- U.S. Postal Service workers
- Public transit workers
- Grocery store workers
1 List could be updated in the future.
IF YOU RECEIVEDJ&J/Janssen COVID-19 Vaccine
People ages 18 years and older who received a J&J/Janssen COVID-19 vaccine at least 2 months ago should get a booster shot. The J&J/Janssen COVID-19 vaccine has lower vaccine effectiveness over time compared to mRNA COVID-19 vaccines (Pfizer-BioNTech and Moderna).
Your Vaccination Card and Booster Shots
At your first vaccination appointment, you should have received a CDC COVID-19 Vaccination Record Card that tells you what COVID-19 vaccine you received, the date you received it, and where you received it. Bring this vaccination card to your booster shot vaccination appointment.
If you did not receive a CDC COVID-19 Vaccination Record Card at your first appointment, contact the vaccination site where you got your first shot or your state health department to find out how you can get a card.
Infections and Spread
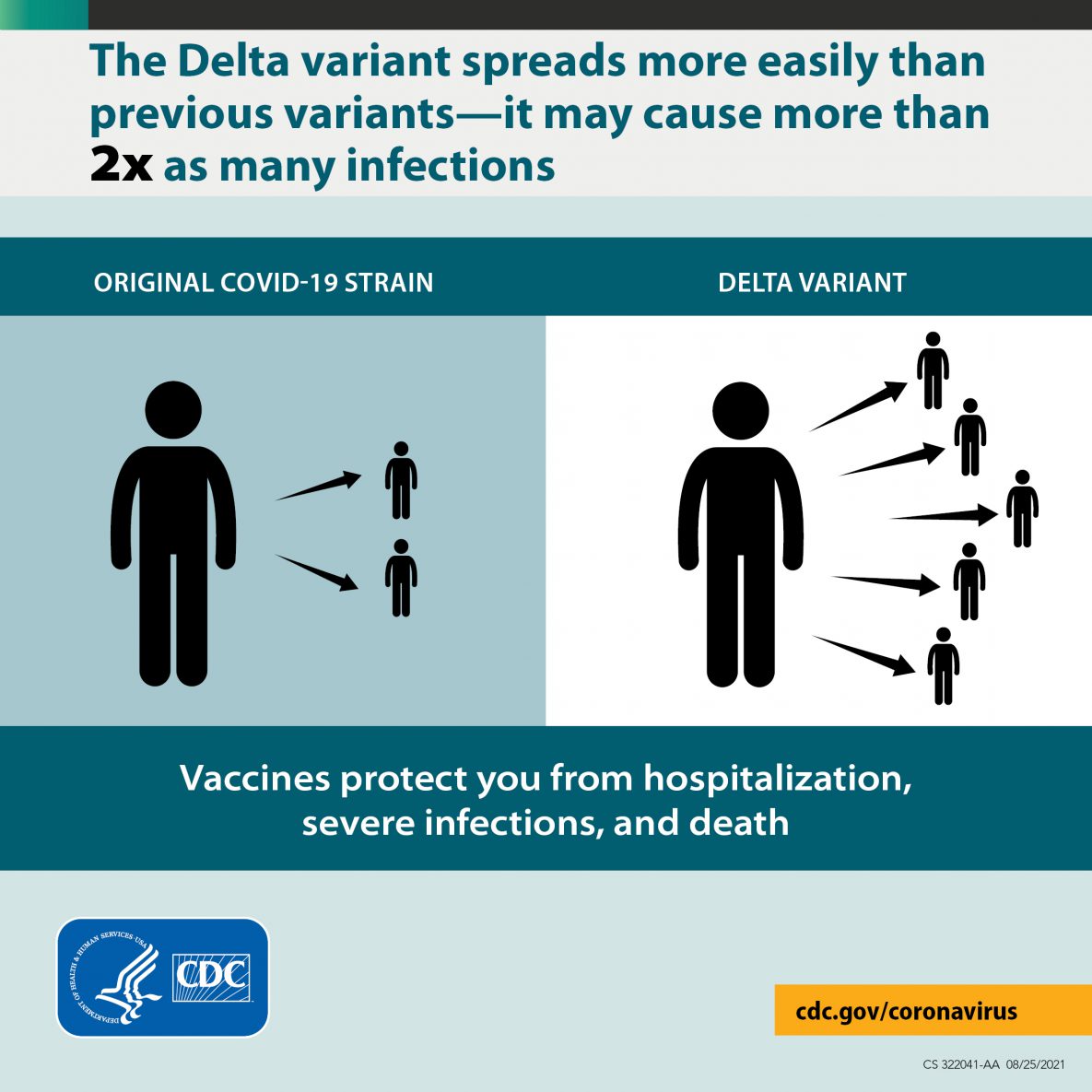
The Delta variant causes more infections and spreads faster than early forms of SARS-CoV-2, the virus that causes COVID-19
- The Delta variant is more contagious: The Delta variant is highly contagious, more than 2x as contagious as previous variants.
- Some data suggest the Delta variant might cause more severe illness than previous variants in unvaccinated people. In two different studies from Canada and Scotland, patients infected with the Delta variant were more likely to be hospitalized than patients infected with Alpha or the original virus that causes COVID-19. Even so, the vast majority of hospitalization and death caused by COVID-19 are in unvaccinated people.
- Unvaccinated people remain the greatest concern: The greatest risk of transmission is among unvaccinated people who are much more likely to get infected, and therefore transmit the virus. Fully vaccinated people get COVID-19 (known as breakthrough infections) less often than unvaccinated people. People infected with the Delta variant, including fully vaccinated people with symptomatic breakthrough infections, can transmit the virus to others. CDC is continuing to assess data on whether fully vaccinated people with asymptomatic breakthrough infections can transmit the virus.
- Fully vaccinated people with Delta variant breakthrough infections can spread the virus to others. However, vaccinated people appear to spread the virus for a shorter time: For prior variants, lower amounts of viral genetic material were found in samples taken from fully vaccinated people who had breakthrough infections than from unvaccinated people with COVID-19. For people infected with the Delta variant, similar amounts of viral genetic material have been found among both unvaccinated and fully vaccinated people. However, like prior variants, the amount of viral genetic material may go down faster in fully vaccinated people when compared to unvaccinated people. This means fully vaccinated people will likely spread the virus for less time than unvaccinated people.
Masks, social distancing and good sanitation practices are still recommended throughout the state.
LAKE COUNTY: During such a trying time for our nation and state, it is more important than ever that Montanans help each other. Below is a list of your local organizations and resources that are here to help you during the COVID-19 outbreak. Many of these organizations can provide services remotely so you can access the help you need from home.
ARLEE – CHARLO – POLSON – RONAN – ST. IGNATIUS
__________________________________________________________________________
Health Care Facilities:
• Polson Health
106 Ridgewater Dr Suite A
Polson, Montana 59860 Phone: (406) 883-3200
https://www.krh.org/krhc/contact-us
• Providence St. Joseph Medical Center
6 13th Ave East Polson, MT 59860
406-883-5680
Maps & Direction
• ST. Luke Community Healthcare
• Clinics: Ronan (406) 676-3600
St. Ignatius (406) 745-2781
Southshore (406) 883-2555
Ridgewater (406) 883-3737
• St Luke Hospital: (406) 676-4441
https://www.stlukehealthcare.org
ADDITIONAL INFORMATION:
• https://lakecountypublichealth.org/health-alert/
_________________________________________________________________________
The listings below are for Lake County and are available to see patients, however, it is suggested to call ahead. Just click on the website for additional information.
Pharmacies:
• Lake County Council on Aging and Transportation- 528 Main St SW Ronan 676-2367
Leave Message to arrange transportation for pickup of RX or other items.
• Polson: Providence St Joseph Pharmacy 6 13th Ave E 883-8444. Free delivery or mail.
Patients please call if RX being picked up by another ID for controlled substances.
• Polson: Credena Health Pharmacy 50331 US Hwy 93 (Super 1) 406-883-0342 Free delivery
or mail. Patients call ahead if RX picked up by another ID for controlled substances.
• Polson: Safeway Pharmacy 1146 South Shore Route 406-883-3674 Free mailing, and free
delivery on T and F only within 10 mile radius.
• Polson: Walmart 36318 Memory Lane 406-883-9221 drive thru and store has 60+
Tuesdays 6-7 am
• Polson: Walgreens 40770 Mount Hwy 35 Polson, MT 406-300-6042 Drive thru. Patient please call
ahead if others picking up RX Tuesdays 8-9 am Seniors only All day Tuesday Seniors 20% off name brand and 30% off Walgreen brand.
• Ronan: Family Health Pharmacy 633307 US 93 Ronan Mt 406-676-2111 drive thru and curbside
• Ronan: R&R Health Care Solutions Pharmacy 63802 US Hwy 93 Ronan Mt 406-676-5600 will deliver within Ronan city limits, will mail, can do curbside if paid with CC in advance.
• ST. Ignatius: Mission Drug 110 N Main St St. Ignatius Mt 406-745-3000 Call ahead for curbside delivery Will mail except controlled substances and NO PO Boxes
Food / Groceries:
• POLSON: Polson Senior Center –504 3rd Ave E Polson, Mt. 406-883-4735 Open and serving To-Go meals M-F 11:45-12:30 Call ahead for meals. Served curbside.
Home Delivered program (Meals on Wheels continues- call for application).
• Mission Mountain Natural Foods – 319 Main St Polson Mt. 406-883-2847 Regular store hours Call ahead for delivery availability. Will do curbside pickup and charge CC but must call and order ahead.
• Walmart Polson: https://www.walmart.com/store/2607/polson-mt
• Super 1 Foods Polson: https://www.super1foods.net/
• Safeway Polson: https://local.safeway.com/safeway/mt/polson/146
• RONAN: Mission Valley Senior Center, 528 Main St SW Ronan, Mt 406-676-2371 Open for
grab and go meals M-W-F call ahead and leave message to be placed on meal schedule for following day.
• Boys and Girls Club: 62579 US 93 Ronan Mt 406-676-5437 Follow them on Facebook
https://www.facebook.com/flatheadbgc/ For additional scheduling and updates
• Harvest Foods: 63802 US Hwy 93, 406-676-3301 No delivery or curbside. Senior
Citizen hours T and Th 6-9 am
• Family Dollar Store: 9 Dayton St SW Ronan 406-552-0859 Patrons can call ahead
and clerk will bring order out to vehicle where they can pay at the vehicle.
• ST IGNATIUS: St Ignatius Senior Center, 212 N Main 406-745-4462 leave message and call ahead to order meals. Take out and Home delivery only.
• Rod’s Harvest Foods: 116 N Main St St Ignatius 406-745-4275 Call ahead and clerk will deliver curbside where you can pay at that time.
Many of the local establishments have set special times for seniors and individuals with disabilities to shop separately from the general public. Additionally, several locations have delivery and curbside pickup for your convenience.
• CHARLO: Charlo Grocery, 55609 Mount Hwy 212 Charlo 644-2575 Will do curbside delivery but must be paid with cash or check .
• ARLEE: Wilson Foods, 92345 US Hwy 93 Arlee 726-7777 Service remains same.
• http://www.polsonchamber.com/takeoutpolson/ (TAKE OUT ESTABLISHMENTS IN OUR AREA)
• Confederated Salish & Kootenai Tribes: Continue to provide essential services with Home Delivered Meals provided through the tribal nutritional sites below. For questions about Elder Services, please call Constance Morigeau at 406-675-2700, Ext. 1381.
• Arlee Tribal Nutrition Site 406-726-3221
• Elmo Tribal Nutrition Site 406-849-5022
• Polson Tribal Nutrition Center 406-883-6877
• Ronan Tribal Nutrition Center 406-676-5495
• St. Ignatius Tribal Nutrition Center 406-745-4240
For Information Only: Not professional advice Disclaimer: If you need specific advice (for example, medical, legal, financial or risk management), please seek a professional who is licensed or knowledgeable in that area. Never give unsolicited personal or financial data out.
Mental Health:
Mental Health Information
Montana 211 (information for a variety of services and volunteering opportunities)Dial 211 or 406-752-8181
State Mental Health Services Bureau 888-866-0328
Western Montana Mental Health Center 406-532-9190
Addiction Treatment Help Line 877-887-5016
Drug Abuse Hotline (24 hrs)800-311-3069
Alcoholics Anonymous 888-607-2000
Montana Mental Health Ombudsman (help navigating system)888-444-9669
For Information Only: Not professional advice Disclaimer: If you need specific advice (for example, medical, legal, financial or risk management), please seek a professional who is licensed or knowledgeable in that area. Never give unsolicited personal or financial data out.
Other Resources:
• https://lakecountypublichealth.org/health-alert/ (COVID 19)
• http://mdt.mt.gov/publictransit/missoula.shtml (Transportation)
• https://www.daines.senate.gov/coronavirus-resources/help-for-montanaseniors (Other resources in the area)
• Helping Hands: P O Box 1094 Polson Jennifer 406-883-8256 Every M & W will drop off groceries, medication call by previous Friday.
• New Life Church: www.newlifepolson.com 1414 2nd St W 406-883-2447 or call 406-304-7013 can assist with different tasks, call for more information.
• Hot Springs City Hall: 109 Main St 406-741-2353 Call for Community Information
• Shepherd of The Valley Lutheran Church: 1192 Mt. Silcox Dr Thompson Falls 406-827-9570 Contacts: Pastor Jacob Berger, Mark and Karen Sheets, Congregation. They are willing to volunteer, and availability will depend on request.
• http://www.polsonchamber.com (Polson Chamber of Commerce)